Dental bone grafting is a procedure that increases the amount of bone in a part of the jaw where bone has been lost or where extra support is necessary. It may involve surgically transferring bone from one part of the body to the existing jawbone. Sometimes, synthetic bone materials may be used.
A dental bone graft may be required if the health of nearby gums and teeth is endangered by bone loss. It can also serve as a prerequisite procedure for further surgical procedures, such as dental implants.
Stay on this page to learn all the basic information about dental bone grafts, the procedure involved, and what to expect or do after getting a dental bone graft.
Also read: 4 Types of Dental Implants: How to Know The Right One For You
What Is a Dental Bone Graft?
Dental bone grafts can be done in several ways. However, they all involve the same basic procedure: an oral surgeon or dentist makes an incision in the jaw and attaches (grafts) another bone material to the jaw.
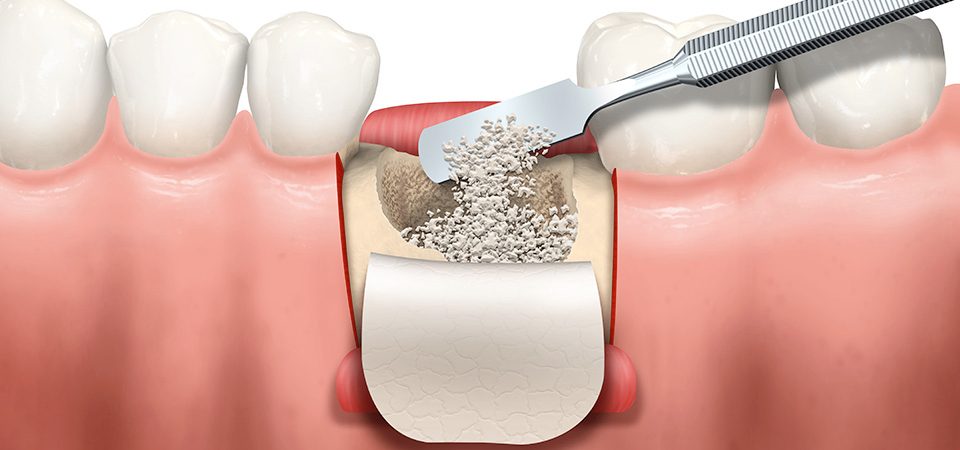
The most preferred bone source for the grafting involves taking part of the patient’s bone from the hip, tibia, or back of the jaw in a process called autografting. However, where autografts are unadvisable, your dental health professional may consider other options: allografts, xenografts, or alloplasts.
In allografts, the dental health professional uses bone from a different person, usually a cadaver. Xenografts involve attaching bone from another species, such as a cow, pig, or coral. With alloplasts, a dentist or oral surgeon attaches synthetic material like calcium phosphate or calcium sodium phosphosilicate (Bioglass) to the jaw region.
Usually, the procedure may be required in people with missing teeth (or teeth) or gum disease. It can also help to fill an empty tooth socket following an extraction or rebuild your jaw before getting dentures.
How to Know I Require Dental Bone Grafting?
Your dental health professional is in the best position to determine whether or not you require a dental bone graft. A dentist or oral surgeon might recommend this procedure if you have:
- Gum disease (Periodontal disease)
- Bone loss
- Scheduled implants for lost teeth
1. Gum disease
Gum disease, if not managed effectively, can lead to bad breath, loose teeth and bleeding, and swollen gums. In extreme cases, it can even cause heart dysfunction. A dentist would suggest a dental bone graft to help stabilize the jaw, prevent spread to nearby teeth and gum tissues, and mitigate other long-term health conditions that come with it.
2. Bone loss
Losing a bone or tooth is a condition that can require you to get a dental bone graft. When you lose bone mass in the jaw, it can cause undesirable changes to your face.
In most cases, the face may appear sunken, the lower part of the face can collapse, and the jawline may become less defined, leading to the appearance of jowls.
To correct this, dental bone grafting is one option most dentists would recommend.
3. Implants for lost teeth
People who have scheduled implants for missing teeth are the most common candidates for dental bone grafts. According to a 2023 study by the University of Minnesota School of Dentistry, nearly 65% of patients scheduled for dental implants require bone augmentation procedures.
This stat reinforces the importance of bone grafts for implants, as it ensures they have a solid foundation and achieve long-term success.
Also read: What is Cantilever Bridge Dental: Here’s All You Must Know in 2025
Preparing for a Dental Bone Graft
There isn’t much preparation required when planning to go for a dental bone graft. However, here are some of the things your dentist will ask you to do before the procedure:
- Brush and floss gently the day before the operation to minimize the risk of infection.
- Avoid eating or drinking anything for about 8 to 12 hours before the procedure. The time would vary depending on the type of anesthesia you receive. So, ask your dentist for certainty.
- Do not take any aspirin products or blood-thinning medications at least three days before your appointment. You might need to confirm with your dentist the medications you should avoid pre-surgery.
What Happens During a Dental Bone Grafting Procedure?
The details of how a dental bone grafting surgery is carried out vary depending on your dentist, the impacted region, and other unique conditions. However, below is a general outline of what happens during a dental bone grafting procedure.
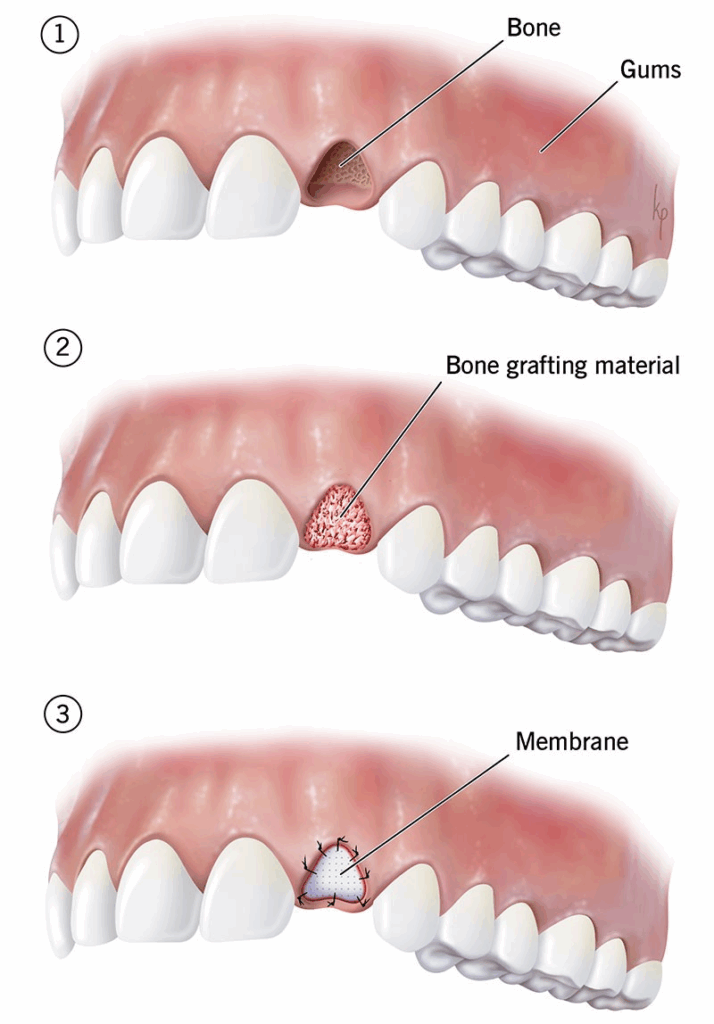
During dental bone grafting, your oral surgeon or dentist will:
- Numb your gums with local anesthetic. If you consent to be put to sleep for surgery, your health provider will also provide you with sedation meds.
- Make an incision (cut) in your gums
- Gently separate your gums from your jawbone
- Clean and disinfect the region
- Add dental bone grafting material to areas of bone loss
- Cover the bone graft with a membrane (also purchased from a tissue bank) to shield it during the healing period. Often, the membrane will absorb and go away on its own during healing. Others don’t, and will require your provider to remove it during a follow-up visit.
- Reposition your gums.
- Close the incision with stitches.
It’s important to note that your healthcare provider may add platelet-rich plasma (PRP) to your dental bone graft. They obtain the PRP from a sample of your blood, and it helps to promote healing and tissue regeneration.
How Painful Is Dental Bone Grafting?
A dental bone graft that doesn’t involve harvesting bone material from a patient’s own body is a relatively minor surgical procedure. Studies show that most patients with a basic dental bone graft experience little to no pain. You only want to ensure that you take all prescribed medications (such as pain medications) and follow your post-op instructions closely.
However, there’s a higher likelihood of pain if you had an autograft (i.e., bone transfer from your own body). That’s because it involves surgery in two locations (your hip and jaw). That said, since the harvested bone amount is usually quite small, the period of discomfort should be brief.
How Do I Recover After a Dental Bone Graft?
Firstly, you should know you’ll likely leave the dentist’s office with your mouth packed with gauze guarding the incision. Your dentist should give you instructions for changing clothes during the next 24 hours and a prescription for antibiotics to help prevent any infection. They may also recommend pain relievers.
Other aftercare tips to note include:
- Eating soft, bland foods for the first few days and avoiding hard or crunchy foods like nuts
- Sleeping with your head slightly elevated over the first two nights to help prevent blood from aggregating around the incision site
- Apply ice packs to help reduce pain and swelling for the first two days.
- Avoiding strenuous physical activities like contact sports that may threaten the incision
- Avoiding drinking hot liquids like coffee or soup
It’s important to note that dental bone grafts have a high success rate, with lower chances of complications developing in most patients. The dull pain in your jaw should give way to mild discomfort after about a week and show signs of improvement.
While your jaw should feel normal after a few weeks, it usually takes a few months before your jaw is strong enough to receive implants. Finally, consider scheduling periodic visits to your dentist, including at least one comprehensive X-ray scan, to check on your healing.
How Expensive Is a Dental Bone Graft?
The cost of a dental bone graft can differ significantly, depending on the complexity of the involved procedure and the material used.
Where a bone graft’s source material is from a cadaver, animal, or synthetic substance, the cost could vary between $400 and $1,200. However, an autograft is more expensive and could cost $2,000 or more.
While most insurance providers don’t cover the entire cost of dental bone grafts, your insurer may cover part of the procedure. However, if you requested a bone graft over cosmetic wants, you’re not likely to receive any insurance coverage.
Also read: Pros and Cons of Having Two Dental Insurance
Conclusion
Dental bone grafts can help prevent long-term health conditions connected with gum disease or tooth loss. They’re usually safe and readily tolerable, but can come with the risk of side effects and complications.
Follow your doctor’s guidance during recovery to reduce your chances of developing problems after the procedure and raise your chances of maintaining good dental health in the coming days.
Consider visiting your doctor if complications develop, such as redness or increased swelling around the gums, loosened implants, or worsened pain days after the procedure.