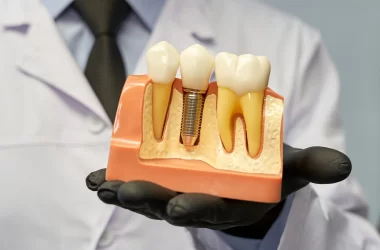
Dental bone grafts help restore the jawbone before implant placement. Bone grafts become necessary when the dental surgeon determines that the jawbone on which the transplant is to be done has lost some volume due to tooth extraction, gum disease, trauma, or long-term tooth absence.
Dental bone grafts create a solid foundation for dental implants, bridges, or dentures, thereby enhancing oral health, function, and aesthetics. Understanding the dental bone graft healing stages is crucial for setting patients’ expectations regarding the recovery required after the procedure. It ensures optimal outcomes.
Our guide is designed as a walkthrough of the intricacies of the bone regeneration process that occurs, from immediately after the procedure until the newly formed bone fully integrates into the jawbone.
Read also: Here’s Everything to Know About Dental Bone Grafting: Is It Right for You?
Why Dental Bone Graft Is Important

A jawbone missing one or more teeth begins to shrink because it no longer receives needed stimulation produced by the lost tooth’s roots during chewing. Over time, the bone loss deforms the face and reduces the jawbone’s ability to obtain and carry an implant.
A dental bone graft reverses the decline by adding volume and density to the site of the loss. Also, it promotes the body’s natural ability to regenerate new bone at the site of the loss.
The graft material—which could be autograft (patient’s bone tissue), allograft (human donor bone tissue), xenograft (animal donor bone tissue), or alloplastic (synthetic material)—acts as a scaffold around and over which new bone regenerates.
Dental Bone Graft Healing Stages
- Stage 1 – Initial Recovery (days 1 – 7)
The healing process after a dental bone graft begins immediately following the procedure. Those first few days are critical for initial clot formation and wound stability.
Clot formation is crucial because it physically seals the surgical wound, preventing it from becoming contaminated with harmful bacteria, which can cause infection and inflammation. Additionally, it promotes healing by providing a scaffold for the growth of new bone and tissue.
Days 1-3 represent the acute postoperative phase. This phase is characterized by swelling and discomfort around the surgical site. Also, bleeding around the surgical site might occur.
Patients are advised to diligently follow their surgeon’s instructions, which may include gently rinsing the mouth periodically with warm salty water, eating only soft foods during the healing process, and avoiding the use of straws of any kind. There is no brushing of the oral cavity during this period.
Applying ice packs intermittently can help alleviate swelling, while medications prescribed by the attending surgeon can help reduce pain.
Days 4 – 7 are the early healing phase. The swelling would have peaked and begun to subside. The blood clot that has formed will continue to mature, eventually developing into a fibrin mesh that serves as a framework for new cell growth.
Patients will continue their oral hygiene regimen using only mouthwashes and special rinses prescribed by the attending surgeon.
- Stage 2 – Soft Tissue Healing (Weeks 2 – 4)
By this phase, the gums around the surgical site would have entirely closed over it, providing the necessary barrier over and around the underlying bone graft. Bone integration (of the graft) begins around this period.
The body recognizes the graft and grows new blood vessels into it. Those blood vessels act as channels for receiving nutrients and specialized cells needed for bone regeneration.
Usually, there is less swelling and improved comfort during this period. There would be no changes to the oral hygiene routines or diet prescribed by the attending surgeon.
- Stage 3 – Vascularization and Early Osteoinduction/Osteoconduction (Months 1 – 2)
This phase of healing marks the point where the actual bone regeneration begins. The biological process is complex, but it results in the complete replacement of the graft material by the recipient’s bone tissue.
During this phase, the graft material serves as a scaffold that guides the growth of new bone through a process known as osteoconduction. Alongside, growth factors in the graft and its surrounding tissues trigger stem cells to begin differentiating into osteoblasts, which are vital bone-forming cells, through a process known as osteoinduction.
The blood supply to and around the surgical site improves, as does the connective tissue matrix within the graft. The graft begins to solidify into a base strong enough to receive and carry subsequent dental prosthetics.
- Stage 4 – Woven Bone Formation (Months 2 – 4)
At this stage, the osteoblasts become more active and begin to lay a groundwork of new, immature bone, known as woven bone. Woven bone increases the structural strength of the graft site.
Additionally, the graft material begins to be broken down or resorbed by osteoclasts as new bone forms in the space. This continuous remodeling is key to the success of the graft.
- Stage 5 – Lamellar Bone Maturation and Remodeling (Months 4 – 6)
This phase of healing entails the gradual transformation of woven bone into the stronger lamellar bone. The lamellar bone is what the adult jawbone is made of.
Remodeling continues, resulting in a graft site that becomes denser and more robust. Also, the graft material is increasingly replaced by native bone. The result will be that the graft site will be sufficiently thick and voluminous.
- Stage 6 – Continued Maturation and Densification (Months 6 – 12)
Healing of the surgical site continues beyond the 6-month mark. The jawbone continues to mature, remodel, and densify. The lamellar bone being formed becomes more organized as it readies itself to receive incoming prosthetics.
- Stage 7 – Long-Term Stability (12 Months and Beyond)
Here, the site of the graft would have fully integrated into the surrounding bone structure and would become indistinguishable. It becomes a stable, solid foundation able to receive and carry implants for several years.
Read also: Here’s How Much Dental Bone Graft Cost Today
Factors That Affect The Healing Timeline

Several factors directly affect the speed and success of the dental bone graft healing stage:
- Type of graft material used
Autografts (the use of the patient’s bone tissue) heal faster and produce more successful outcomes because of their biological compatibility. Other types of graft materials—allografts, xenografts, and alloplasts—also offer good results for the most part, but they integrate over a slightly longer timeline.
- The size of the graft and its location
The larger a dental bone graft is, the longer it takes to heal. Additionally, if the dental bone graft is located in an area with a less abundant blood supply, it may take a longer time to heal.
- The Recipient’s Overall Health
The patient’s overall health is a crucial factor in determining the healing timeline of a dental bone graft. For example, a patient who has diabetes or an autoimmune disorder will take longer to heal from the procedure.
- Smoking
Smoking negatively impacts the healing timeline. Smoking reduces the necessary blood flow and thus hinders bone regeneration. That slows down the healing process and increases the risk of complications.
- Poor Oral Hygiene
A dental bone graft requires meticulous cleaning to prevent bacterial infection of the site. It will take longer to heal if the recipient is negligent in following the attending dentist’s postoperative oral hygiene instructions.
- Strict Compliance With the Postoperative Instructions Issued By the Dental Surgeon
The healing timeline is also influenced by the degree to which the patient adheres to the dental surgeon’s postoperative instructions regarding diet, activity, and medication.
- Nutrition
The timely intake of food and prescribed supplements containing vital nutrients can help accelerate the healing process. For example, vitamins D and K, as well as calcium and phosphorus, are known to support bone formation.
Possible Complications That May Arise From A Dental Bone Graft
Dental bone graft procedures are safe, although they may occasionally lead to unexpected complications. Understanding the potential complications that could arise is part of the preparation required for the dental bone graft healing stages.
- Infection
An infection in the surgical site can be caused by bacteria that are usually present in the mouth. Such an infection will be characterized by persistent pain, moderate to severe swelling, the presence of pus, or fever.
- Graft Exposure
The graft material could become exposed through the gum tissue.
- Nerve Damage
Nerve damage can be characterized by temporary or permanent numbness in the surgical site. This injury rarely occurs.
- Graft Failure
This failure happens when the recipient’s body refuses to integrate the bone graft or outrightly rejects it.
Any complication following a dental bone graft procedure requires the immediate attention of the attending dental surgeon. Most complications can be recognized through excessive bleeding, prolonged pain, or swelling at the surgical site.
Read also: 50 Soft Foods to Eat After Dental Surgery
Conclusion
The dental bone graft healing stages illustrate the regenerative capabilities of the human body. Every stage—from the formation of the blood clot to the final fusion of the new bone formed into the jawbone—contributes to the success of the procedure.
Patience is an important attribute that would help recipients of dental bone grafts, as it empowers them to be active participants in the healing process. It will also help patients stick to the strict postoperative oral hygiene and dietary regimen required for a successful dental bone graft outcome.
That successful outcome is the stable, durable base that paves the way for subsequent restorative treatments. Also, there is a vast improvement in the oral health and quality of life of the recipient.
It’s best to always consult with board-certified dental professionals for advice and care regarding any planned dental bone grafts.